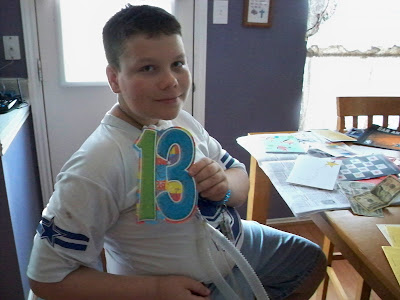from Friday, May 12, 2006 11:02AM
My favorite "Mother" Story
I was asked to enter a writing contest
by submitting my favorite "mother" story.
The prize was a nice gift certificate to Bath & Body.
Whether I win that prize or not was not
that important to me.
But the message in the story
and the feelings in it,
I am happy to share.
I thought I would now share it with all of you.
Read below:
My young son looks up at me,
his blue eyes shining,
but his mouth unable to emit words.
A tube down his throat, taped at his top lip
gets in the way
so even though he is moving his mouth
to say the words, I cannot make them out.
He so desperately wants me to understand him;
and we both feel like I should, I am his mother.
But no matter how frantically
I try to come up with guesses,
I just cannot figure out
what he is trying to say.
Maybe he could write something to me –
but he hasn’t learned to spell many words,
and his hand is bound, so even that doesn’t help.
In fact, it only makes it worse;
he becomes more frustrated
and tears form in his eyes.
If only he could get up out of his bed
to go get an object
to help me understand.
What could be worse
than to have tubes in your mouth
and nostrils, IV's attached to your arms,
having to wear diapers
far beyond potty training years
and you can't even get your own mother
to understand your needs?
That describes many days my son and I faced
in the weeks leading up to his 9th birthday –
a day we would mark in isolation
in the pediatric intensive care unit in the hospital.
That birthday seemed like it would be our most dreary
and depressing – because my son
would not be able to have any of his friends
or much of his family around him.
He would not yet be able to eat cake
or even be free of all the tubes
binding him to his hospital bed.
Those days in the hospital,
I cried so many tears –
as I thought of the party I did not get to plan for him,
and all the things I was sure he was feeling.
But the only time I would let myself cry
was when I knew he was sleeping
or I went into another room.
I was so busy being so strong for him,
but inside, I was crumbling.
The day of his birthday finally arrived.
His nurses and hospital staff tried their very best
to make Josh smile.
They brought him gifts, balloons and decorations.
They sang to him and promised a cake the moment
he could eat some.
Then, our church family got into the act –
they collected money and taped it to a giant card.
They brought that plus bags and bags of gifts for him.
He probably got more birthday presents this year
than he got in the last five altogether!
And we got to throw him a party
a few weeks later
once we got home.
We combined the occasions –
getting to come home from the hospital
with his belated birthday and
invited friends and family and
we all enjoyed ourselves.
And for this party –
to make sure there was enough –
we baked four cakes!
What makes this story my favorite, as a mother,
was to see just how well my son accepted
such terrible medical circumstances,
to feel the love so many people showered upon us
and the one on one time I got to spend
with my son that would not have been possible otherwise.
I will always cherish that time,
despite the difficulties.
I hope that story blesses you like it does me.
Have a wonderful day!
Vanessa
Thursday, September 24, 2009
Tuesday, September 22, 2009
breaking down ROHHAD
ROHHAD stands for
Rapid Onset Obesity with
Hypothalamic Dysfunction,
Hypoventilation and
Autonomic Dysregulation
Whenever someone asks what Joshua has, it is sure a mouthfull to give the full name of the diagnosis.. but that is it.
So, let's break it down and give some definitions and examples, to help everyone better understand it.
Rapid Onset Obesity
seems pretty self explanatory
you gain a great deal of weight very quickly even when you don't suddenly begin overeating, etc.
Hypothalamic dysfunction
Overview
Hypothalamic dysfunction is a problem with the region of the brain called the hypothalamus, which helps control the pituitary gland and regulate many body functions.
Symptoms
Symptoms generally relate to the hormones that are missing. In children, there may be growth problems -- either too much growth or too little -- or puberty that occurs too early or too late.
Tumor symptoms:
Headaches, Loss of vision
Hypothyroidism symptoms:
Breast enlargement, Cold intolerance, Fatigue,
Hair or skin changes, Impotence,
Loss of body hair and muscle (in men),
Menstrual disturbance, Weight gain
Low adrenal function symptoms:
Dizziness, Weakness
Other, less common symptoms may include:
Body temperature disturbance,
Emotional abnormalities, Excess thirst,
Obesity, Uncontrolled urination
Kallmann's syndrome (a type of hypothalamic dysfunction that occurs in men) symptoms:
Lowered function of sexual hormones (hypogonadism)
Inability to smell
Treatment
Treatment depends on the cause of the hypothalamic dysfunction.
Tumors -- surgery or radiation
Hormonal deficiencies -- replace missing hormones
Specific treatments may be available for bleeding, infection, and other causes.
Causes
The hypothalamus helps control the pituitary gland, particularly in response to stress. The pituitary, in turn, controls the:
Adrenal glands, Ovaries, Testes, Thyroid gland
The hypothalamus also helps regulate:
Body temperature, Childbirth, Emotions,
Growth, Milk production, Salt and water balance,
Sleep, Weight and appetite
Causes of hypothalamic dysfunction include:
Anorexia, Bleeding, Bulimia,
Genetic disorders, Growths (tumors),
Head trauma, Infections and swelling (inflammation).
Malnutrition, Radiation, Surgery, Too much iron
The most common tumors in the area are craniopharyngiomas in children.
Tests & diagnosis
Blood or urine tests to determine levels of hormones such as:
Cortisol, Estrogen, Growth hormone,
Pituitary hormones, Prolactin,
Testosterone, Thyroid
Other possible tests:
Hormone injections followed by timed blood samples,
MRI or CT scans of the brain,
Visual field eye exam (if there is a tumor)
Prognosis
Many causes of hypothalamic dysfunction are treatable. Most of the time missing hormones can be replaced.
Prevention
Maintain a healthy diet and don't exercise too strenuously or lose weight too quickly. If you believe you have an eating disorder such as anorexia or bulimia, get medical attention: these conditions can be life-threatening.
If you have symptoms of a hormonal deficiency, discuss replacement therapy with your health care provider.
Complications
Complications of hypothalamic dysfunction depend on the cause.
Brain tumors:
Permanent blindness
Specific problems related to the brain area where the tumor occurs
Vision disorders
Hypothyroidism:
Heart problems
High cholesterol
Adrenal insufficiency:
Inability to deal with stress (such as surgery or infection)
Gonadal deficiency:
Heart disease
Impotence (in men)
Infertility
Thin bones (osteoporosis)
Growth hormone deficiency:
High cholesterol
Osteoporosis
Short stature (in children)
Weakness
When to contact a doctor
Call your doctor if you have:
Headaches
Symptoms of hormone excess or deficiency
Vision problems
Hypoventilation
from Wikipedia
In medicine, hypoventilation (also known as respiratory depression) occurs when ventilation is inadequate[1] (hypo means "below") to perform needed gas exchange. By definition it causes an increased concentration of carbon dioxide (hypercapnia) and respiratory acidosis.
Causes
It can be caused by medical conditions, such as stroke affecting the brain stem, by holding one's breath, or by drugs, typically when taken in overdose.
Effects
As a side effect of medicines or recreational drugs, hypoventilation may become potentially life-threatening. Many different CNS depressant drugs such as alcohol, benzodiazepines, barbiturates, GHB, sedatives and opiates produce respiratory depression when taken in large or excessive doses; however this is most commonly seen as a cause of death with opiates or opioids, particularly when they are combined with sedatives such as alcohol or benzodiazepines. Strong opiates, (fentanyl, heroin, morphine, etc), barbiturates, and the benzodiazepine, temazepam, are notorious for producing this effect; in an overdose, an individual may cease breathing entirely (go into respiratory arrest) which is rapidly fatal without treatment.
Treatment
Respiratory stimulants such as nikethamide were traditionally used to counteract respiratory depression from CNS depressant overdose, but were of only limited effectiveness. A new respiratory stimulant drug BIMU8 is currently being investigated which seems to be significantly more effective and may be useful for counteracting the respiratory depression produced by opiates and similar drugs without offsetting their therapeutic or recreational effects.
Associated conditions
Disorders referred to as "Congenital Central Hypoventilation Syndrome" or "CCHS" and "Rapid-Onset Obesity, Hypothalamic Dysfunction, Hypoventilation, with Autonomic Dysregulation" or ROHHAD are recognized. CCHS condition may be a significant factor in some cases of sudden infant death syndrome or SIDS, often termed "cot death" or "crib death."
The opposite condition is hyperventilation (too much ventilation), resulting in low carbon dioxide levels (hypocapnia), rather than hypercapnia.
Autonomic Dysregulation
from http://www.drmueller-healthpsychology.com/autonomic_dysregulation.html
What is Autonomic Dysregulation?
The autonomic nervous system controls most of the involuntary reflexive activities of the human body. The system is constantly working to regulate the glands and many of the muscles of the body through the release or uptake of the neurotransmitters acetylcholine and norepinephrine. The autonomic nervous system is made up of two primary parts: the sympathetic and parasympathetic systems.
The sympathetic nervous system prepares the body for emergencies or times of stress and is responsible for the body's "fight or flight" response when faced with a dangerous situation. During this response, the heart rate and blood pressure increase, the pupils of the eye dilate, and the digestive system slows down.
The parasympathetic system helps the body's functions return to normal after they have been stimulated by the sympathetic nervous system and also has some responsibility for keeping the body's immune system properly functioning.
Autonomic dysregulation involves malfunctioning of the autonomic nervous system, the portion of the nervous system that conveys impulses between the blood vessels, heart, and all the organs in the chest, abdomen, and pelvis and the brain (mainly the medulla, pons and hypothalamus).
Here is an article I found about a treatment for Hypothalamic Dysfunction
Immunoglobulin Therapy in Idiopathic Hypothalamic Dysfunction
Peter Huppke, MD, Alexander Heise, MD†, Kevin Rostasy, MD‡, Brenda Huppke, MD
Received 19 January 2009; accepted 18 March 2009.
Idiopathic hypothalamic dysfunction is a rare disorder presenting at age 3-7 years. Severe hypothalamic and brainstem dysfunction leads to death in 25% of patients. The disease is presumed to be autoimmune, or in some cases paraneoplastic. No successful treatment has been reported. Patient V. developed hyperphagia, hypersomnia, and extreme aggression at age 7 years, accompanied by episodes of hyperthermia, hypothermia, sinus bradycardia, hypernatremia, hyponatremia, persistent hyperprolactinemia, hypothyroidism, and growth-hormone deficiency. At age 9 years, a diagnosis of idiopathic hypothalamic dysfunction was rendered, and immunoglobulin therapy was commenced. Nine courses of immunoglobulins, at a dose of 2 g/kg every 4 weeks, were administered. Reproducible improvements in behavior and no further episodes of hyponatremia or hypernatremia and sinus bradycardia were evident. The endocrinologic abnormalities and poor thermoregulation remained. Administration of immunoglobulins during late stages of idiopathic hypothalamic dysfunction led to improvement in some but not all signs. Assuming an autoimmune basis for this disorder, treatment during early stages of disease should be more effective. To facilitate such early treatment, increased awareness of this disorder is necessary, to allow for early diagnosis.
Department of Pediatrics and Pediatric Neurology, Georg August University, Göttingen, Germany
† Department of Child and Adolescent Psychiatry, Georg August University, Göttingen, Germany
‡ Division of Pediatric Neurology, Department of Pediatrics, Medical University of Innsbruck, Innsbruck, Austria
Communications should be addressed to: Dr. Huppke; Department of Pediatrics and Pediatric Neurology; Faculty of Medicine, Georg August University; Robert-Koch-Strasse 40; D-37075 Göttingen, Germany.
PII: S0887-8994(09)00163-5
doi:10.1016/j.pediatrneurol.2009.03.017
© 2009 Elsevier Inc. All rights reserved.
Rapid Onset Obesity with
Hypothalamic Dysfunction,
Hypoventilation and
Autonomic Dysregulation
Whenever someone asks what Joshua has, it is sure a mouthfull to give the full name of the diagnosis.. but that is it.
So, let's break it down and give some definitions and examples, to help everyone better understand it.
Rapid Onset Obesity
seems pretty self explanatory
you gain a great deal of weight very quickly even when you don't suddenly begin overeating, etc.
Hypothalamic dysfunction
Overview
Hypothalamic dysfunction is a problem with the region of the brain called the hypothalamus, which helps control the pituitary gland and regulate many body functions.
Symptoms
Symptoms generally relate to the hormones that are missing. In children, there may be growth problems -- either too much growth or too little -- or puberty that occurs too early or too late.
Tumor symptoms:
Headaches, Loss of vision
Hypothyroidism symptoms:
Breast enlargement, Cold intolerance, Fatigue,
Hair or skin changes, Impotence,
Loss of body hair and muscle (in men),
Menstrual disturbance, Weight gain
Low adrenal function symptoms:
Dizziness, Weakness
Other, less common symptoms may include:
Body temperature disturbance,
Emotional abnormalities, Excess thirst,
Obesity, Uncontrolled urination
Kallmann's syndrome (a type of hypothalamic dysfunction that occurs in men) symptoms:
Lowered function of sexual hormones (hypogonadism)
Inability to smell
Treatment
Treatment depends on the cause of the hypothalamic dysfunction.
Tumors -- surgery or radiation
Hormonal deficiencies -- replace missing hormones
Specific treatments may be available for bleeding, infection, and other causes.
Causes
The hypothalamus helps control the pituitary gland, particularly in response to stress. The pituitary, in turn, controls the:
Adrenal glands, Ovaries, Testes, Thyroid gland
The hypothalamus also helps regulate:
Body temperature, Childbirth, Emotions,
Growth, Milk production, Salt and water balance,
Sleep, Weight and appetite
Causes of hypothalamic dysfunction include:
Anorexia, Bleeding, Bulimia,
Genetic disorders, Growths (tumors),
Head trauma, Infections and swelling (inflammation).
Malnutrition, Radiation, Surgery, Too much iron
The most common tumors in the area are craniopharyngiomas in children.
Tests & diagnosis
Blood or urine tests to determine levels of hormones such as:
Cortisol, Estrogen, Growth hormone,
Pituitary hormones, Prolactin,
Testosterone, Thyroid
Other possible tests:
Hormone injections followed by timed blood samples,
MRI or CT scans of the brain,
Visual field eye exam (if there is a tumor)
Prognosis
Many causes of hypothalamic dysfunction are treatable. Most of the time missing hormones can be replaced.
Prevention
Maintain a healthy diet and don't exercise too strenuously or lose weight too quickly. If you believe you have an eating disorder such as anorexia or bulimia, get medical attention: these conditions can be life-threatening.
If you have symptoms of a hormonal deficiency, discuss replacement therapy with your health care provider.
Complications
Complications of hypothalamic dysfunction depend on the cause.
Brain tumors:
Permanent blindness
Specific problems related to the brain area where the tumor occurs
Vision disorders
Hypothyroidism:
Heart problems
High cholesterol
Adrenal insufficiency:
Inability to deal with stress (such as surgery or infection)
Gonadal deficiency:
Heart disease
Impotence (in men)
Infertility
Thin bones (osteoporosis)
Growth hormone deficiency:
High cholesterol
Osteoporosis
Short stature (in children)
Weakness
When to contact a doctor
Call your doctor if you have:
Headaches
Symptoms of hormone excess or deficiency
Vision problems
Hypoventilation
from Wikipedia
In medicine, hypoventilation (also known as respiratory depression) occurs when ventilation is inadequate[1] (hypo means "below") to perform needed gas exchange. By definition it causes an increased concentration of carbon dioxide (hypercapnia) and respiratory acidosis.
Causes
It can be caused by medical conditions, such as stroke affecting the brain stem, by holding one's breath, or by drugs, typically when taken in overdose.
Effects
As a side effect of medicines or recreational drugs, hypoventilation may become potentially life-threatening. Many different CNS depressant drugs such as alcohol, benzodiazepines, barbiturates, GHB, sedatives and opiates produce respiratory depression when taken in large or excessive doses; however this is most commonly seen as a cause of death with opiates or opioids, particularly when they are combined with sedatives such as alcohol or benzodiazepines. Strong opiates, (fentanyl, heroin, morphine, etc), barbiturates, and the benzodiazepine, temazepam, are notorious for producing this effect; in an overdose, an individual may cease breathing entirely (go into respiratory arrest) which is rapidly fatal without treatment.
Treatment
Respiratory stimulants such as nikethamide were traditionally used to counteract respiratory depression from CNS depressant overdose, but were of only limited effectiveness. A new respiratory stimulant drug BIMU8 is currently being investigated which seems to be significantly more effective and may be useful for counteracting the respiratory depression produced by opiates and similar drugs without offsetting their therapeutic or recreational effects.
Associated conditions
Disorders referred to as "Congenital Central Hypoventilation Syndrome" or "CCHS" and "Rapid-Onset Obesity, Hypothalamic Dysfunction, Hypoventilation, with Autonomic Dysregulation" or ROHHAD are recognized. CCHS condition may be a significant factor in some cases of sudden infant death syndrome or SIDS, often termed "cot death" or "crib death."
The opposite condition is hyperventilation (too much ventilation), resulting in low carbon dioxide levels (hypocapnia), rather than hypercapnia.
Autonomic Dysregulation
from http://www.drmueller-healthpsychology.com/autonomic_dysregulation.html
What is Autonomic Dysregulation?
The autonomic nervous system controls most of the involuntary reflexive activities of the human body. The system is constantly working to regulate the glands and many of the muscles of the body through the release or uptake of the neurotransmitters acetylcholine and norepinephrine. The autonomic nervous system is made up of two primary parts: the sympathetic and parasympathetic systems.
The sympathetic nervous system prepares the body for emergencies or times of stress and is responsible for the body's "fight or flight" response when faced with a dangerous situation. During this response, the heart rate and blood pressure increase, the pupils of the eye dilate, and the digestive system slows down.
The parasympathetic system helps the body's functions return to normal after they have been stimulated by the sympathetic nervous system and also has some responsibility for keeping the body's immune system properly functioning.
Autonomic dysregulation involves malfunctioning of the autonomic nervous system, the portion of the nervous system that conveys impulses between the blood vessels, heart, and all the organs in the chest, abdomen, and pelvis and the brain (mainly the medulla, pons and hypothalamus).
Here is an article I found about a treatment for Hypothalamic Dysfunction
Immunoglobulin Therapy in Idiopathic Hypothalamic Dysfunction
Peter Huppke, MD, Alexander Heise, MD†, Kevin Rostasy, MD‡, Brenda Huppke, MD
Received 19 January 2009; accepted 18 March 2009.
Idiopathic hypothalamic dysfunction is a rare disorder presenting at age 3-7 years. Severe hypothalamic and brainstem dysfunction leads to death in 25% of patients. The disease is presumed to be autoimmune, or in some cases paraneoplastic. No successful treatment has been reported. Patient V. developed hyperphagia, hypersomnia, and extreme aggression at age 7 years, accompanied by episodes of hyperthermia, hypothermia, sinus bradycardia, hypernatremia, hyponatremia, persistent hyperprolactinemia, hypothyroidism, and growth-hormone deficiency. At age 9 years, a diagnosis of idiopathic hypothalamic dysfunction was rendered, and immunoglobulin therapy was commenced. Nine courses of immunoglobulins, at a dose of 2 g/kg every 4 weeks, were administered. Reproducible improvements in behavior and no further episodes of hyponatremia or hypernatremia and sinus bradycardia were evident. The endocrinologic abnormalities and poor thermoregulation remained. Administration of immunoglobulins during late stages of idiopathic hypothalamic dysfunction led to improvement in some but not all signs. Assuming an autoimmune basis for this disorder, treatment during early stages of disease should be more effective. To facilitate such early treatment, increased awareness of this disorder is necessary, to allow for early diagnosis.
Department of Pediatrics and Pediatric Neurology, Georg August University, Göttingen, Germany
† Department of Child and Adolescent Psychiatry, Georg August University, Göttingen, Germany
‡ Division of Pediatric Neurology, Department of Pediatrics, Medical University of Innsbruck, Innsbruck, Austria
Communications should be addressed to: Dr. Huppke; Department of Pediatrics and Pediatric Neurology; Faculty of Medicine, Georg August University; Robert-Koch-Strasse 40; D-37075 Göttingen, Germany.
PII: S0887-8994(09)00163-5
doi:10.1016/j.pediatrneurol.2009.03.017
© 2009 Elsevier Inc. All rights reserved.
Monday, September 21, 2009
Joshua's 13th Birthday (party slideshow)
I put together a great slideshow of Joshua's 13th Birthday party.
For some reason, though, when I try to embed that slideshow here on my blog, it does not want to show the correct slideshow. In fact, it takes somebody else's slideshow and inserts it here. I have no idea why.
For some reason, though, when I try to embed that slideshow here on my blog, it does not want to show the correct slideshow. In fact, it takes somebody else's slideshow and inserts it here. I have no idea why.
I did get the slideshow to show up on my MySpace blog.
You can see it at this website:
http://blogs.myspace.com/index.cfm?fuseaction=blog.view&friendId=50554238&blogId=511083705
Or see the slideshow on RockYou.com where I made it: http://www.rockyou.com/show_my_gallery.php?source=ppsl&instanceid=153167811
There are some great pictures on there not only of Josh
Or see the slideshow on RockYou.com where I made it: http://www.rockyou.com/show_my_gallery.php?source=ppsl&instanceid=153167811
There are some great pictures on there not only of Josh
and his friends who were able to come to the party,
but of his sister, Steff (who is 23 weeks pregnant)
and her husband & his mother.
We have some folks we'd like to say
We have some folks we'd like to say
a special thank you to...
PAPA JOHN'S PIZZA on FM 3009 in Schertz... for donating 8 pizzas for Joshua's party

HEB BAKERY at I-35 and FM 3009 in Schertz... for donating a full sheet sized cake for Joshua's party

PARTY CITY in the Forum Shopping Center at I-35 & Loop 1604 in Selma/Live Oak... for donating a balloon bouquet for the party.

STARBUCKS on I-35 in Schertz for donating a Frappacino & large cookie to Josh for his birthday


If you get a chance, visit these businesses
and make sure to tell them thank you from us
when you drop by.
Oh, and thank you Nurse Nancy for arranging for all the donations!
You all helped make Joshua's birthday the best one yet!!!
Oh, and thank you Nurse Nancy for arranging for all the donations!
You all helped make Joshua's birthday the best one yet!!!
Saturday, September 19, 2009
Joshua's 13th Birthday (pre-party)
That's right, Josh is now 13!
Love them Grandmas :)
Josh got a box full of goodies today at the post office.
They come from a special group: Aspen Dental from Syracuse, New York
here's a GREAT BIG THANKS TO the folks from ASPEN DENTAL!!!!
Spurs Trash Can (and notice the toothbrushes)
A Spurs Penant
A Dallas Cowboys blanket and Hat
an issue of Sports Illustrated from January 24, 1972
featuring the Dallas Cowboys WOW!!
and a huge thanks to HEB for donating a full sheet sized cake for Josh's birthday party!!!!
Amanda and Nurse Nancy fixed Josh up with some stuff for his Wii
(Nurse Nancy even made the calls to arrange for the cake, several pizzas from Papa John's and a dozen balloons from Party City - Nancy is one sweet nurse!!!!!!)
Amanda got Josh this fishing game for Josh
this was Josh the day before his birthday... sleeping on the couch for several hours... he had to really gear up for his big day, you know!
His party is tonight from 5-7 at Neimeitz Park in Cibolo. He already has footballs, baseballs, basketball and even frisbee ready to take over to play with his guests with. I'll update with pictures from the party, etc. later.
Thursday, September 17, 2009
Moving Day for Daughter
September 15, 2009
My daughter has been married one month this day!
We're still waiting on all those professional pictures to be edited and ready for us :( I can't wait to get them... but I guess I'll have to.
On this day, even though Steff was sick with a respiratory infection not to mention being 5 months pregnant, it was when she and new hubby Bryan were to move into their new apartment.
She decided she kind of needed her Mom to help out (smile). So, Josh, his nurse and I drove over to lend a hand.
We stayed busy for hours carrying stuff down from the upstairs apartment to the new place.
We didn't finish everything that first day, so the next morning, I came over again (after Josh went to school). I worked on scrubbing the kitchen and shampooing the carpets in the old upstairs apartment. And together, Steff and I got their new place a bit more organized.
Here's a quick glance at her new home:

check out that baby bump!!!!

living room

Kitchen
After we called it a day, I took Steff to lunch....

her choice.... McDonalds
My daughter has been married one month this day!
We're still waiting on all those professional pictures to be edited and ready for us :( I can't wait to get them... but I guess I'll have to.
On this day, even though Steff was sick with a respiratory infection not to mention being 5 months pregnant, it was when she and new hubby Bryan were to move into their new apartment.
She decided she kind of needed her Mom to help out (smile). So, Josh, his nurse and I drove over to lend a hand.
We stayed busy for hours carrying stuff down from the upstairs apartment to the new place.
We didn't finish everything that first day, so the next morning, I came over again (after Josh went to school). I worked on scrubbing the kitchen and shampooing the carpets in the old upstairs apartment. And together, Steff and I got their new place a bit more organized.
Here's a quick glance at her new home:

check out that baby bump!!!!

living room

Kitchen
After we called it a day, I took Steff to lunch....

her choice.... McDonalds
Friday, September 11, 2009
Josh Fundraiser
My son, Joshua (you remember him -
he's the one with the super rare disorder, on a ventilator
with a trach in his neck) is trying to sell the most items
in his school's fundraiser.

You can help him by doing a little shopping online.
CLICK THIS LINK TO SHOP FOR JOSH WOOTEN
 .
.
Every item you buy gives points to Josh
so he can win a really great prize.
His goal is to win an ipod.
He needs your help, though.
Did I mention his 13th birthday is next week, Sept. 19th.
You can consider it your birthday gift to him.
Thanks!!!!!!
he's the one with the super rare disorder, on a ventilator
with a trach in his neck) is trying to sell the most items
in his school's fundraiser.

You can help him by doing a little shopping online.
CLICK THIS LINK TO SHOP FOR JOSH WOOTEN
Every item you buy gives points to Josh
so he can win a really great prize.
His goal is to win an ipod.
He needs your help, though.
Did I mention his 13th birthday is next week, Sept. 19th.
You can consider it your birthday gift to him.
Thanks!!!!!!
Monday, September 7, 2009
New Sonogram Pictures of Grandbaby & Josh birthday party plans plus ROHHAD recap
Steffany & Baby
I picked up the sonogram pictures my daughter, Steffany had at her last appointment. She is about 21 weeks along here, which is a little early to be sure of the sex of the baby, but they do point out "it looks like a boy".... check out the pictures below:





Steffany and the baby are reportedly in good health so that is great news!
Joshua & Pacers
Meanwhile, Joshua is doing well but still has to wait awhile longer before we get to start up those breathing pacemakers. His lung doctor wants to get a face to face meeting with the makers of the pacers to make sure he (and his staff) are ready to oversee us with them. He promises it will be soon and we can't wait!
Joshua's birthday (SEPTEMBER 19th) is coming up soon and we are looking at probably having his party at the park like we did last year. We just hope this time there is no car wreck (remember last year, my sister, her boyfriend Nick and Steffany were involved in an accident on their way to deliver the birthday cake. Luckily none of them was badly hurt.)
PICTURES FROM JOSHUA'S LAST BIRTHDAY PARTY (SEPT 2008)






This year, Joshua really wants an IPOD.


The one he's heard about is the Touch. But it is super duper expensive, so he's been saving up his money and gift cards in hopes that he can afford one. I'd rather he pick something cheaper. I'd hate for him to save all that money and then have the thing break on him or lose it. I'll bet I can talk him into a cheaper gadget that does most of the same stuff. And as long as he gets to play some sports with his buddies, he will have a terrific time at his party. He is such a good sport!
ROHHAD Recap
I realize there are some folks new to us who come across us and do not know about Joshua's medical problems, so I'd like to take a few moments and explain a bit about ROHHAD.

Joshua was about as healthy and normal as a kid could be from birth up to around 8 and a half years old, when he suddenly without explanation became very tired (lethargic) and his fever shot up.






I took him to a minor emergency clinic where a doctor discovered his blood oxygen level was half what it should be. The doctor put him on oxygen and rushed him by ambulance to a hospital, where he was admitted and ended up in the pediatric intensive care unit. Hours after being admitted, Joshua went into respiratory arrest and had to be revived 5 times then hooked to a ventilator with a hose/tube down his mouth and throat.

Numerous tests failed to show what caused the near fatal incident. But during the time in ICU, Joshua also experienced paralysis of his left arm and leg, then a seizure. Powerful steroids (IV IG) was used to get Joshua strong enough to come off the ventilator and regain his sensations in his left side. He was released with only outpatient therapies. But a few months later, Joshua's blood oxygen level started dropping again and he was re-admitted to another hospital. Again, he had to be put on a ventilator and tests done. And again, tests did not show what caused the problem.
Josh stayed in the hospital with a tube in his mouth down his throat for weeks so he could be properly ventilated while doctors searched for the cause of his troubles. Finally, after the doctors reached out online for help from anyone worldwide, they had a response. A doctor in Chicago had seen a similar case and helped make a diagnosis. It was called Late-Onset Central Hypoventilation Syndrome with Hypothalamic Dysfunction. There was no known cause for it and thus no known cure.
But it appeared Joshua would need to have some help with ventilation for likely the rest of his life. So, the doctors asked us to consider having a tracheostomy tube surgically placed in his neck so he could hook to a ventilator without having to have a tube through his mouth. That way, he could eat, drink, talk and move around better. Joshua underwent surgery to place the "trach" tube three days before his 9th birthday, September 16th, 2005. He remained in the hospital a couple more weeks, healing from his surgery and giving us time to become educated about caring for him with a trach and being on a ventilator.




At this time, his doctors thought he really only needed to be ventilated when he slept or got really sick. So, he spent the days unhooked, but with his ventilator very near by just in case. And then at night, we would carry up his ventilator to be at his bedside and hook him up at bedtime. And Joshua's doctor wanted him to have a specially trained nurse to be at his side for him to go to school, since we who had training to care for him would not be with him there. So, he was homebound for a couple of months until the school could hire and specially train a nurse for him.
We thought back then that the doctor who helped diagnose him in Chicago would get us in to see her in a short time and see if he would be a candidate to recieve special breathing pacemakers. Our doctor here read up on them and was very hopeful they would be the solution to our problem. And the doctor in Chicago had recommended them for some of her patients and worked with them afterwards. So, we waited to get in to see her. That wait was an entire year! But finally, we got word of an appointment date, and we were so excited!

Since I had not been able to work a normal job since Josh was hospitalized the 2nd time, our finances were really poor. But I was determined to get Josh in to see the doctor in Chicago somehow. I found a program through Southwest Airlines to get our travel arranged, and we got there. It was a long and grueling week of testing, but we were so pumped. We just knew it would end with Josh getting his pacemakers and he could be free of his trach and ventilator in a matter of a few short months. But that was not to be.
The doctor never mentioned pacemakers that whole week. And when I finally asked her, "well, is Joshua a candidate for the pacemakers? When do we find out about them?" She looked at me like I was crazy. She had no intention of pacemakers for Josh - at least not in the near future. She was only confirming his diagnosis and checking to make sure his ventilator was working properly for him. We were devastated. And we couldn't understand how there could be that big a miscommunication between doctors.



Back home, our doctor here was excited to hear about our visit. She too thought we'd be coming back with great news of pacemakers. And she was very disappointed that they were not even being looked at as an option. One main thing that came from our time in Chicago is that Joshua was now expected to be on his ventilator pretty much 24 hours a day! He really was not breathing big enough breaths ever on his own to keep his oxygen levels up and get rid of enough carbon dioxide (CO2). So, now we had 2 ventilators - one for bedside and one to carry around with us everywhere we went.
I was at a loss for how we were going to have Josh carry around a heavy ventilator all the time - especially if he had to go to the bathroom all of a sudden or something. So, I searched for a buggy or cart of somekind that was designed to hold up a ventilator - and found NOTHING. So, I ended up having to fashion one for him myself. That was fun. We had to make sure there was enough weight at the right places to keep the cart from falling over. And we had to have plug ins for the ventilator and other monitors he'd need, and places to put all his medical supplies. We've gone through two different styles of carts now and our current one is pretty good but is sure a catch-all for Joshua's junk. He likes to put a deck of cards in, and his pencils, pens, highlighters, hearing aids, sunglasses, and pretty much anything he might have in his hands when he's wanting to walk out the door. Keeping all that stuff from falling out is the trick now.



But we did actually FINALLY find a doctor who would consider the breathing pacemakers for Joshua. This doctor was in Houston - much closer to us. But first, Josh had to undergo lots more testing by all that doctor's colleagues. They wanted to make sure there wasn't some other diagnosis we might be missing - something that could be fixed another way.

That took several more months. But I figured it would be worth it if they found they could fix his problems some other way. They finally decided they had no better answers and got him scheduled for the surgery for diaphragmatic pacemakers in June 2009.

He is finally healed up and ready to start using the pacers but Joshua's new lung doctor here has never had patients with these devices and he's a bit nervous about being in charge of them. So, we're waiting on him to prepare himself and his staff.
Oh, I forgot to mention that the doctor who saw Josh way back in 2006 in Chicago, used his information along with a few others to get an article published about his disorder. In it, she and another doctor changed the name of the disorder to ROHHAD (Rapid-Onset Obesity With Hypothalamic Dysfunction, Hypoventilation, and Autonomic Dysregulation Presenting in Childhood).
The disorder involves more than just the shallow breathing and not sensing the problem. It also caused Josh to stop producing growth hormones. So I give him nightly injections of human growth hormones. He gets one night off a week. He also sweats heavily at times and gets dehydrated terribly easily without explanation. He takes DDAVP for that. It is in the form of a nose spray. It causes him to retain fluids. And his body does not regulate temperature as it should. So, we have to be careful about him getting too hot or too cold. I don't know if it's directly related or was caused by brain damage when he wasn't getting enough oxygen, but Joshua also has a pretty serious learning delay and a high frequency hearing loss in both ears. I have learned to give Joshua certain vitamin supplements and lots of fluids to try and help keep him balanced and hopefully improve his memory and brain function.
So, that's it in a nutshell - everything you wanted to know about Josh and his ROHHAD disorder. Oh, and he was featured in that hour-long documentary that aired on Discovery Channel and Discovery Health. That is at the bottom of my page here, if you want to go back and watch it.
I picked up the sonogram pictures my daughter, Steffany had at her last appointment. She is about 21 weeks along here, which is a little early to be sure of the sex of the baby, but they do point out "it looks like a boy".... check out the pictures below:





Steffany and the baby are reportedly in good health so that is great news!
Joshua & Pacers
Meanwhile, Joshua is doing well but still has to wait awhile longer before we get to start up those breathing pacemakers. His lung doctor wants to get a face to face meeting with the makers of the pacers to make sure he (and his staff) are ready to oversee us with them. He promises it will be soon and we can't wait!
Joshua's birthday (SEPTEMBER 19th) is coming up soon and we are looking at probably having his party at the park like we did last year. We just hope this time there is no car wreck (remember last year, my sister, her boyfriend Nick and Steffany were involved in an accident on their way to deliver the birthday cake. Luckily none of them was badly hurt.)
PICTURES FROM JOSHUA'S LAST BIRTHDAY PARTY (SEPT 2008)






This year, Joshua really wants an IPOD.


The one he's heard about is the Touch. But it is super duper expensive, so he's been saving up his money and gift cards in hopes that he can afford one. I'd rather he pick something cheaper. I'd hate for him to save all that money and then have the thing break on him or lose it. I'll bet I can talk him into a cheaper gadget that does most of the same stuff. And as long as he gets to play some sports with his buddies, he will have a terrific time at his party. He is such a good sport!
ROHHAD Recap
I realize there are some folks new to us who come across us and do not know about Joshua's medical problems, so I'd like to take a few moments and explain a bit about ROHHAD.

Joshua was about as healthy and normal as a kid could be from birth up to around 8 and a half years old, when he suddenly without explanation became very tired (lethargic) and his fever shot up.






I took him to a minor emergency clinic where a doctor discovered his blood oxygen level was half what it should be. The doctor put him on oxygen and rushed him by ambulance to a hospital, where he was admitted and ended up in the pediatric intensive care unit. Hours after being admitted, Joshua went into respiratory arrest and had to be revived 5 times then hooked to a ventilator with a hose/tube down his mouth and throat.

Numerous tests failed to show what caused the near fatal incident. But during the time in ICU, Joshua also experienced paralysis of his left arm and leg, then a seizure. Powerful steroids (IV IG) was used to get Joshua strong enough to come off the ventilator and regain his sensations in his left side. He was released with only outpatient therapies. But a few months later, Joshua's blood oxygen level started dropping again and he was re-admitted to another hospital. Again, he had to be put on a ventilator and tests done. And again, tests did not show what caused the problem.
Josh stayed in the hospital with a tube in his mouth down his throat for weeks so he could be properly ventilated while doctors searched for the cause of his troubles. Finally, after the doctors reached out online for help from anyone worldwide, they had a response. A doctor in Chicago had seen a similar case and helped make a diagnosis. It was called Late-Onset Central Hypoventilation Syndrome with Hypothalamic Dysfunction. There was no known cause for it and thus no known cure.
But it appeared Joshua would need to have some help with ventilation for likely the rest of his life. So, the doctors asked us to consider having a tracheostomy tube surgically placed in his neck so he could hook to a ventilator without having to have a tube through his mouth. That way, he could eat, drink, talk and move around better. Joshua underwent surgery to place the "trach" tube three days before his 9th birthday, September 16th, 2005. He remained in the hospital a couple more weeks, healing from his surgery and giving us time to become educated about caring for him with a trach and being on a ventilator.




At this time, his doctors thought he really only needed to be ventilated when he slept or got really sick. So, he spent the days unhooked, but with his ventilator very near by just in case. And then at night, we would carry up his ventilator to be at his bedside and hook him up at bedtime. And Joshua's doctor wanted him to have a specially trained nurse to be at his side for him to go to school, since we who had training to care for him would not be with him there. So, he was homebound for a couple of months until the school could hire and specially train a nurse for him.
We thought back then that the doctor who helped diagnose him in Chicago would get us in to see her in a short time and see if he would be a candidate to recieve special breathing pacemakers. Our doctor here read up on them and was very hopeful they would be the solution to our problem. And the doctor in Chicago had recommended them for some of her patients and worked with them afterwards. So, we waited to get in to see her. That wait was an entire year! But finally, we got word of an appointment date, and we were so excited!

Since I had not been able to work a normal job since Josh was hospitalized the 2nd time, our finances were really poor. But I was determined to get Josh in to see the doctor in Chicago somehow. I found a program through Southwest Airlines to get our travel arranged, and we got there. It was a long and grueling week of testing, but we were so pumped. We just knew it would end with Josh getting his pacemakers and he could be free of his trach and ventilator in a matter of a few short months. But that was not to be.
The doctor never mentioned pacemakers that whole week. And when I finally asked her, "well, is Joshua a candidate for the pacemakers? When do we find out about them?" She looked at me like I was crazy. She had no intention of pacemakers for Josh - at least not in the near future. She was only confirming his diagnosis and checking to make sure his ventilator was working properly for him. We were devastated. And we couldn't understand how there could be that big a miscommunication between doctors.



Back home, our doctor here was excited to hear about our visit. She too thought we'd be coming back with great news of pacemakers. And she was very disappointed that they were not even being looked at as an option. One main thing that came from our time in Chicago is that Joshua was now expected to be on his ventilator pretty much 24 hours a day! He really was not breathing big enough breaths ever on his own to keep his oxygen levels up and get rid of enough carbon dioxide (CO2). So, now we had 2 ventilators - one for bedside and one to carry around with us everywhere we went.
I was at a loss for how we were going to have Josh carry around a heavy ventilator all the time - especially if he had to go to the bathroom all of a sudden or something. So, I searched for a buggy or cart of somekind that was designed to hold up a ventilator - and found NOTHING. So, I ended up having to fashion one for him myself. That was fun. We had to make sure there was enough weight at the right places to keep the cart from falling over. And we had to have plug ins for the ventilator and other monitors he'd need, and places to put all his medical supplies. We've gone through two different styles of carts now and our current one is pretty good but is sure a catch-all for Joshua's junk. He likes to put a deck of cards in, and his pencils, pens, highlighters, hearing aids, sunglasses, and pretty much anything he might have in his hands when he's wanting to walk out the door. Keeping all that stuff from falling out is the trick now.



But we did actually FINALLY find a doctor who would consider the breathing pacemakers for Joshua. This doctor was in Houston - much closer to us. But first, Josh had to undergo lots more testing by all that doctor's colleagues. They wanted to make sure there wasn't some other diagnosis we might be missing - something that could be fixed another way.

That took several more months. But I figured it would be worth it if they found they could fix his problems some other way. They finally decided they had no better answers and got him scheduled for the surgery for diaphragmatic pacemakers in June 2009.

He is finally healed up and ready to start using the pacers but Joshua's new lung doctor here has never had patients with these devices and he's a bit nervous about being in charge of them. So, we're waiting on him to prepare himself and his staff.
Oh, I forgot to mention that the doctor who saw Josh way back in 2006 in Chicago, used his information along with a few others to get an article published about his disorder. In it, she and another doctor changed the name of the disorder to ROHHAD (Rapid-Onset Obesity With Hypothalamic Dysfunction, Hypoventilation, and Autonomic Dysregulation Presenting in Childhood).
The disorder involves more than just the shallow breathing and not sensing the problem. It also caused Josh to stop producing growth hormones. So I give him nightly injections of human growth hormones. He gets one night off a week. He also sweats heavily at times and gets dehydrated terribly easily without explanation. He takes DDAVP for that. It is in the form of a nose spray. It causes him to retain fluids. And his body does not regulate temperature as it should. So, we have to be careful about him getting too hot or too cold. I don't know if it's directly related or was caused by brain damage when he wasn't getting enough oxygen, but Joshua also has a pretty serious learning delay and a high frequency hearing loss in both ears. I have learned to give Joshua certain vitamin supplements and lots of fluids to try and help keep him balanced and hopefully improve his memory and brain function.
So, that's it in a nutshell - everything you wanted to know about Josh and his ROHHAD disorder. Oh, and he was featured in that hour-long documentary that aired on Discovery Channel and Discovery Health. That is at the bottom of my page here, if you want to go back and watch it.
Subscribe to:
Posts (Atom)
Discovery Documentary - Life or Death : Battling to Breathe
>